Story
It’s Time to Bring Awareness to Brain Cancer
One in three people in the UK knows someone affected by a brain tumour. This disease is indiscriminate—it can affect anyone, at any age. Brain tumours continue to kill more children and adults under the age of 40 than any other cancer. Yet, since records began in 2002, just 2% of the national cancer research budget has been allocated to this devastating disease.
That is over three decades of underfunding.
If funding were increased, it would give patients and families a fighting chance—accelerating research, improving treatments, and opening access to clinical trials that could save lives.
Imagine working closely with a colleague in the same Directorate — even in the same team — who is a long term survivor of a brain tumour, only for your own husband to collapse with the very same condition. That is what happened to me. Both Paul and I are sharing our personal stories, and at the same time I am hosting a coffee morning in our workplace to raise vital funds for the charity.
Claire's Story:

My name is Claire Brown, and on 31 March 2025, my husband Alex, aged 52, became one of the many people affected by a brain tumour.
Alex’s symptoms developed gradually: fatigue, severe headaches, vision issues, and cognitive changes. Eventually, his tumour grew so large that it increased the pressure in his skull, causing him to collapse in our family home. After seeking advice from our GP, we were told to attend A&E. After a 12-hour wait and a CT scan, we received the devastating news—Alex had a brain tumour, later diagnosed as Astrocytoma Grade 4.
Before his diagnosis, Alex worked 5-6 days a week as a painter and decorator. We have three daughters, aged 27, 15, and 12. The emotional impact on our family is impossible to fully capture: the overwhelming shock, the grief for the life you thought you had, the constant uncertainty, and the quiet, relentless fear of what the future might hold.
The Journey
Sixty percent of brain tumours are diagnosed in A&E — often when patients present in acute crisis.
Alex’s symptoms had worsened rapidly. Over two years, despite multiple GP visits, his symptoms were repeatedly attributed to stress and anxiety. We were incredibly fortunate that the A&E doctor chose to order a CT scan. That single decision changed everything.
Doctors pushed for an urgent MRI, but the specialist neuro oncology team who needed to review it met only once a week. Every day without answers felt unbearable.
Instead of being given a bed, Alex spent two days lying on a hospital corridor. When he was finally admitted, we waited another ten days for the MRI he urgently needed — not because his case wasn’t serious, but because the system was overwhelmed. And without that scan, no one could tell us what was happening inside his brain. Was it cancer? Was it treatable? Were we losing precious, irreversible time?
The waiting was unimaginable torture.
To keep him stable, Alex was placed on high dose steroids and anti seizure medication to reduce the pressure in his skull and prevent further complications. After the MRI, the Ulster Hospital sent us home to wait for an appointment with a neurosurgeon in the Royal. All we knew was that he had a brain tumour that was suspected to be malignant.
Once home, everything became even harder. The medication began to affect his mind, and he experienced episodes of psychosis. We watched his physical and mental health deteriorate, yet we had nowhere to turn — we had been discharged, and neither the GP nor the hospital could offer support. The medication made Alex feel so unwell that he started refusing doses, and I was terrified. We had already been warned that the pressure in his skull could cause a brain bleed and that missing or reducing his medication was dangerous.
I have never felt so helpless or afraid.
It was another two weeks before we finally met the neurosurgeon at the Royal Victoria Hospital. Nothing could have prepared us for what she told us. The tumour was malignant, incurable, and believed to be a high grade mass that had been developing and transforming for some time. Surgery was offered — not as a cure, but to debulk the tumour and give Alex the best possible chance of stability.
We were shown his scans for the first time, and the reality was overwhelming. The tumour was the size of a tennis ball — approximately 7.5 × 5 cm — a life threatening mass dominating the left side of his brain. We were warned that surgery carried significant risks, including permanent brain damage and even death.
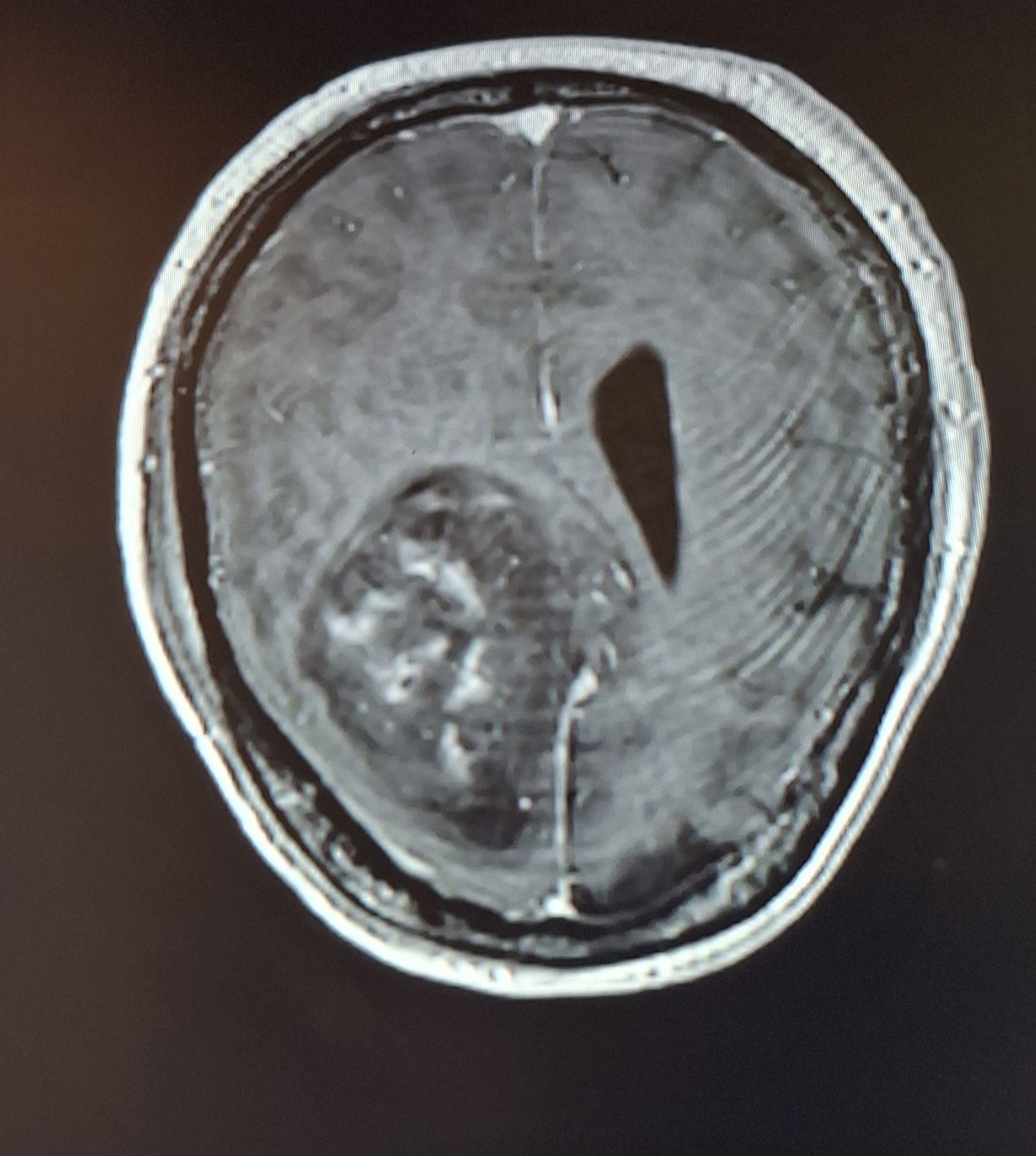
She was so concerned about Alex that she re admitted him immediately. She cancelled her leave—despite it being the Easter weekend—and promised to carry out emergency surgery. She needed a couple of days and further scans to plan the safest way to operate. It was a devastating transition: to go straight from an appointment where we were told he couldn’t be cured, to a neuro ward with no privacy—six beds to a bay—that was horrifying to see. Patients who were brain injured, post surgery, and seriously ill surrounded us. Knowing that this could soon be us was deeply distressing.
Despite the surroundings, the staff, patients, and families we met were just like us — frightened, hopeful, and doing their best to cope. They surrounded us with compassion, support, and a kindness that helped soften some of the fear we were both feeling.
Leaving the hospital that day without Alex again, I was utterly devastated. I felt shocked, overwhelmed, and—if I’m honest—traumatised. I had held it all in, not wanting him to see me fall apart. The moment I reached the car I broke down sobbing and even vomited from the sheer panic of imagining life without my husband. Our whole family had been waiting for reassurance, hoping—just as we were—that the tumour could be removed and cured.
Instead, I had to walk through the door and tell them something very different. I found myself trying to reassure our family that the surgeon would do everything she could, even though inside I was terrified and felt completely alone. I couldn’t believe this was happening to us.
Surgery
On 23 April 2025, Alex underwent an emergency six hour craniotomy at the Royal Victoria Hospital. The tumour was in the left frontal lobe — the area that controls speech, mobility, personality, and so many of the things that make someone who they are.
The wait was unbearable. I sat there wondering if he would survive, if he would ever walk or talk again, if he would still be my Alex when the surgery was over.
Remarkably, the surgeon was able to remove 90% of the tumour — far more than anyone expected. She didn’t just perform an operation; she saved his life and gave us precious time.
Alex woke with 42 staples and a scar stretching from ear to ear. His face was swollen and badly bruised. When I first saw him in ICU, it took a few seconds to even recognise him. I was relieved beyond words — but terrified to touch him, afraid I might hurt him if I tried to hug him. Instead, I squeezed his hand, smiled, and told him I loved him.
Just five days later, he was allowed home — bruised, battered, and looking like he’d gone a few rounds with Mike Tyson and lost badly. After nearly a month in hospitals, I had missed him terribly, especially the simple moments you never think to treasure: walking our dog Gus together, hearing him come through the door after a day’s work, or sitting with a cup of tea in the evening talking about nothing and everything.
The best way I can describe his changes after surgery is this: Alex was a 10 before; he’s now a 7 — for now. But we will forever be grateful to his surgeon. She gave us more time. She gave us hope.
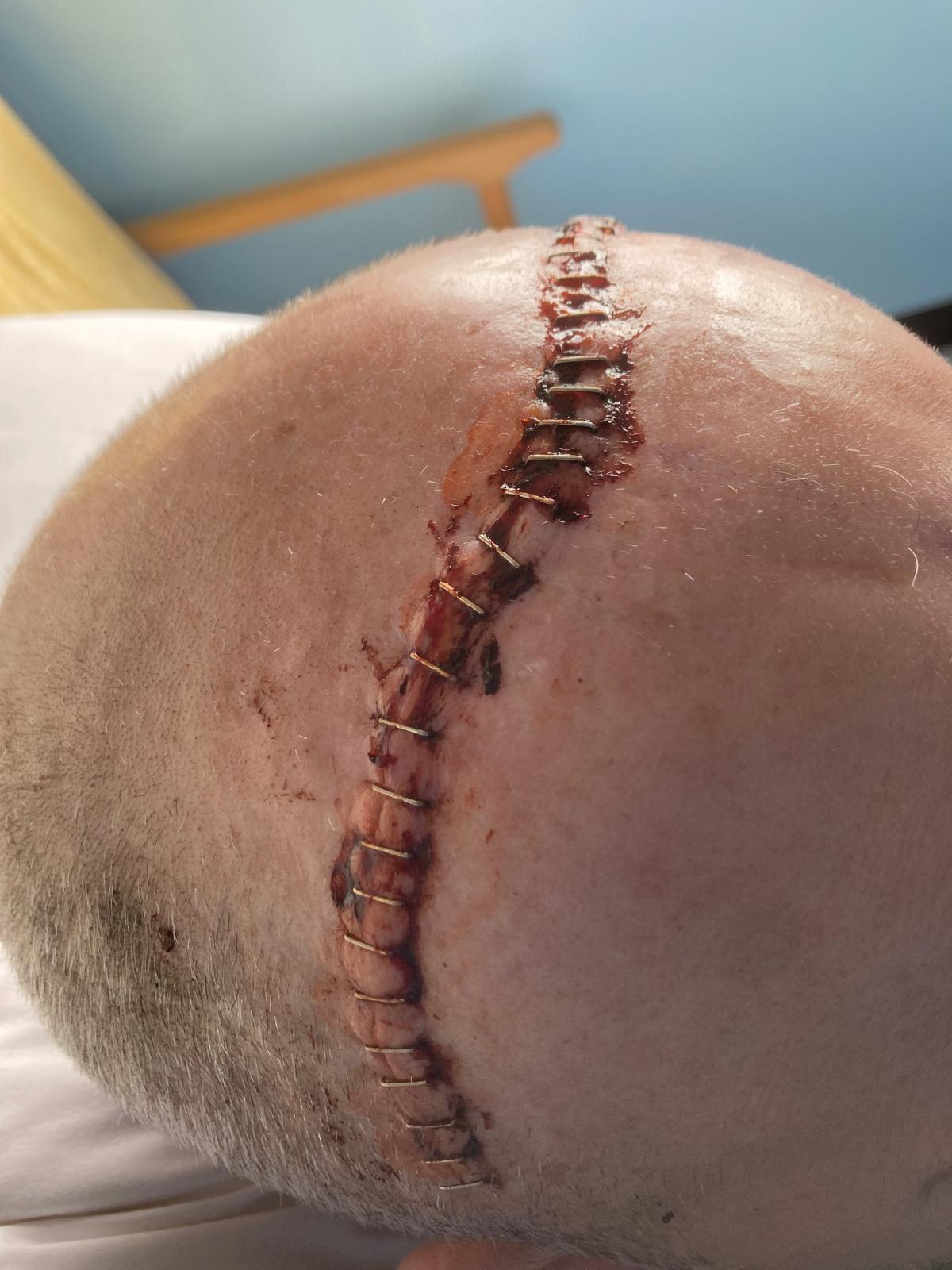
Treatment and Reality
Five weeks later, Alex began radiotherapy and chemotherapy. Overnight, our lives became a relentless cycle of appointments, scans, fatigue, nausea, and difficult side effects. We didn’t even know his exact tumour type until 24 hours before treatment started, because his biopsy had been sent to London for specialist testing—a process that took four agonising weeks. Knowing that some tumour types have better prognoses than others made the wait almost unbearable. We begged for the results over the phone because we couldn’t face another torturous wait outside a consultation room to hear our fate. I had still been holding on to a little hope that it might be a low grade tumour—a grade 1 or 2, something not as bad as they feared. Hearing the real result—a grade 4, and not the tumour type we had hoped for—felt like receiving devastating news all over again.
The chemotherapy Alex receives is the only drug the NHS offers for his tumour type — and it hasn’t changed in more than 35 years. It even carries a risk of secondary cancer, yet it remains his only NHS option. We explored other treatments, but the costs are far beyond our reach, and no clinical trials are available to him because of the postcode lottery. It often feels as though every door is closed before we can even try to open it.
And then there’s the scanxiety — the fear that grips you before every MRI, knowing the future could change in an instant. For now, Alex’s cancer is stable, and we are grateful for every single day. The statistics are terrifying — only 13% of adults with a high grade brain tumour reach five years — but Alex has already shown a determination far stronger than any number. In my heart, I believe he will go further than anyone expects. Northern Ireland may have some of the toughest outcomes, with limited access to trials and new treatments, but we hold on to hope every single day.
Life After Diagnosis
Physically and mentally, this journey has been brutal for Alex. He has had to give up work, surrender his driving licence, and cope with psychiatric, emotional, and cognitive changes that most people will never see. He is not “fine,” even when he tries so hard to appear that way — and I am so incredibly proud of him for the strength and courage he shows every single day.
Our finances changed overnight, but support from the Macmillan finance team and my Civil Service sick pay policy were absolute lifelines when we needed them most.
Through all of this, our children have shown remarkable resilience. I tried to balance caring for Alex, spending long days and nights in the hospital, supporting the younger girls at home and at school, and somehow finding the strength to return to work. I could never have managed without the unwavering support of our family, friends, and colleagues, who carried us through with their kindness, practical help, and constant compassion.
This diagnosis changed everything, yet every day of Alex’s “bonus life” is cherished beyond measure. He is my absolute rock — I cannot imagine life without him, and I love him more than words can ever express.
Why We’re Sharing This
For too long, brain tumour symptoms have been dismissed, misunderstood, or overlooked. Families like ours are left to navigate fear, confusion, and life changing news that might have looked very different if action had come sooner.
We find ourselves asking why—after paying into the NHS and working all our lives—we cannot access the treatment we know could help. It may not be a cure, but it could give us something truly precious: time. Because the treatment we need isn’t available to us here, we’ve been left searching for whatever options we can manage ourselves. We cannot afford the immunotherapy that offers the greatest hope, so we’re turning to a basic, low cost treatment option instead. And because it isn’t an NHS recognised protocol, doctors here cannot prescribe it or offer any support. No family should ever be forced into making these kinds of decisions just to have a chance at more time together, especially when more effective treatments are accessible elsewhere.
Brain tumours are the least survivable cancer, yet they receive some of the lowest levels of research funding. This imbalance is not only heartbreaking — it’s unacceptable.
We speak up because families should not have to rely on luck or perfect timing. We want earlier detection, better treatments, and a healthcare system that gives people a genuine chance.
We need:
• Earlier detection
• Increased research funding
• New and more effective treatments
• Equal access to clinical trials
On Friday 27 February 2026, the Rare Cancers Bill passed its Third Reading in the House of Lords without amendment. It now moves to Royal Assent and will officially become law in the coming weeks. We hope it will bring real, transformative change for people affected by brain tumours, and we have supported its passage through Parliament. For us, this change cannot come soon enough.
By sharing our story, we hope to raise awareness and push for the urgent change that is so desperately needed. We hope that raising awareness will help others recognise symptoms sooner and encourage more support for vital research.
Our lives depend on it.
Paul’s Story:

My name is Paul Bryans and I have been employed within the NICS since 2003. I currently work in the Department of Education. On the 12 August 2017 I learned that I had a terminal Oligodendroglioma brain tumour, which obviously devastated me, my wife and my whole family.
I first noticed something was wrong in April 2017 when I was trying to speak to a friend but lost my balance, was very disorientated and couldn’t speak properly. I gathered my thoughts and went back to have the conversation where I was informed that when I was trying to speak it wasn’t coming out correctly.
The next time this ‘episode’ as I called it, happened when I had just finished in the gym and was waiting for my wife coming out. I started to hear music, and I checked and my car radio was not on. It is hard to explain but at that time I felt really strange, as if I was having an out of body experience. I know that sounds really strange, but that is what was happening to me at the time. I was also not able to speak at times, although I could hear people speaking to me I could not form the sentence I was hearing, and could not speak to answer.
I visited my local GP as I was very concerned about my health, and the episodes were now happening on a regular basis. I was given different suggestions by four different GP’s but after five months of continually bombarding my GP with phone calls they finally sent me for an MRI scan, which confirmed I had a brain tumour.
My Journey
Once the tumour was confirmed on 12 August 2017, everything moved quickly. I began a series of consultations with doctors, consultants, surgeons and speech therapists to put the necessary arrangements in place. My surgery was scheduled for Monday, 4 September 2017, at the Royal Hospital in Belfast.
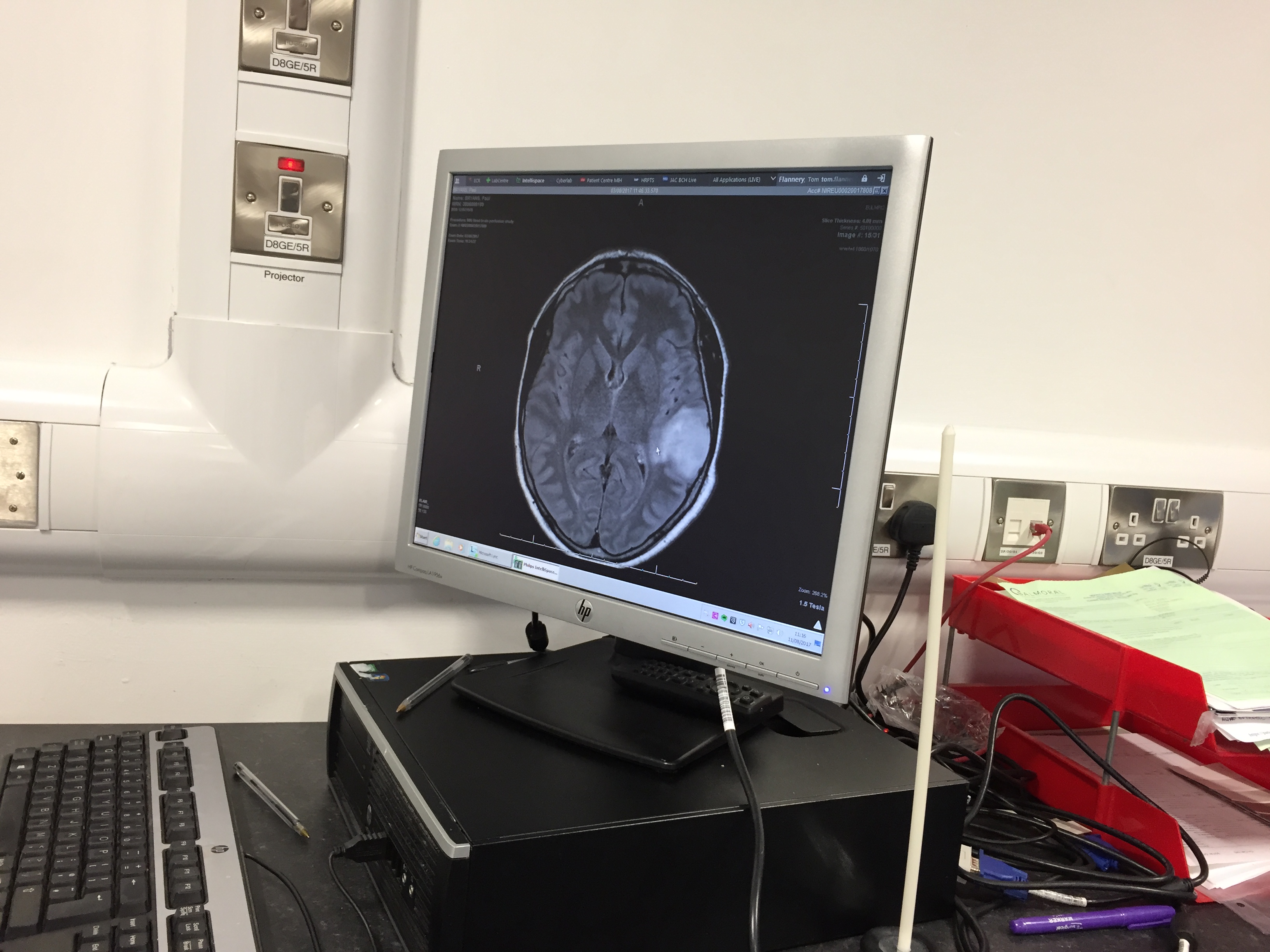
As I continued to experience these episodes — or seizures, as they were medically described — I was not allowed to drive. This meant I had to rely on my wife, Kelly, who had to take time off work to bring me where I needed to be. I was also prescribed medication to help manage the seizures in the period leading up to my surgery.
Obviously, my family and I were distraught at the news I had received but there was nothing we could do until the date for the surgery, which was a very tough and nervous time for everyone.
At the time the Royal Hospital was struggling for beds so I was not even sure I would be getting a bed for my surgery. On Saturday 3 September I received a call for the hospital to confirm a bed was available for me but I had to go straight away and stay in the hospital to secure my bed. Although I was glad to get the bed, this was two days before my surgery, and this only added to the stress for me and my family.
On the Sunday night, the night before my surgery, the surgeon came to visit me at 10.30pm to explain what would be happening the next morning.
Surgery
On Monday, 4 September 2017, I didn’t sleep much the previous night. I was given medication and gowns and everything needed before surgery. I spoke to my family before the porter wheeled me to the operation theatre. I had to be awake for this surgery (awake craniotomy) so I was given enough medication to numb the pain, although I felt a lot of pain I think I shouldn’t have had to feel.
The surgery lasted 3.5 hours, then wheeled to the recovery unit for observation for another 2 hours. I just wanted to speak to my wife and family so I asked the surgeon if he would let them know that the surgery had finished, which he did.
Eventually, I returned to my ward where I was able to spend time with my wife and family. When I was speaking to my wife I was able to tell her in great detail about everything that had happened, what I could see and what I felt throughout the surgery.
That night I was not allowed any medication for the pain regarding the surgery, and I was woken every hour to check my blood pressure etc. A very long night would follow and when the surgeon came to see me, I asked if I could go home to recover as I felt well enough to go and they could use my bed for someone else. After I had been taken for an MRI and results were given to me, I was told they had removed just over 70% of the tumour but I would have to wait a further week or two to see the results of the tumour.
I was told that I could go home if I thought I was well enough. After being told that I could wake up from the surgery with limited sight, hearing, speech and movement and be in hospital for ten days, I was very happy to leave and go home.
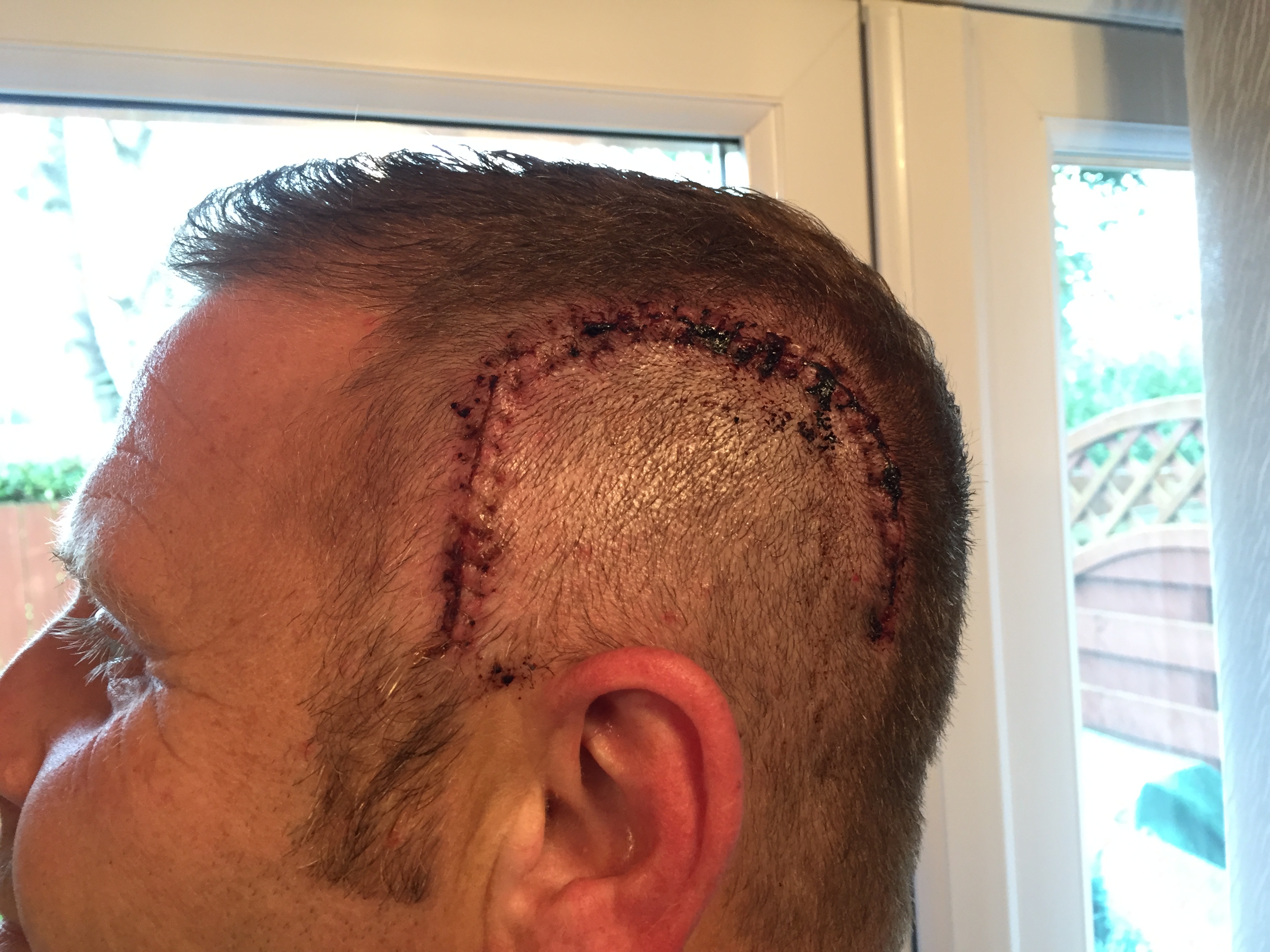
Treatment
My wife and I were called up to the Royal Hospital one week later for my results. I am usually a positive person, but I had a bad feeling about this visit, which turned out to be correct. My wife and I were told I had brain cancer and this could be managed but not cured. I asked for a time frame, but they were unable to give one at that stage. They told me that if the tumour came back, they could operate again. We were absolutely devastated leaving the hospital that day.
On the positive side, I was able to get treatment which I know that so many people do not get that opportunity.
Eight weeks after the surgery I started radiotherapy, every day for six weeks. It was tiring at times, but it had to be done so my wife and I got stuck in it and got it done. No side effects really, apart from losing my hair and sleeping more than I used to.
I finished my radiotherapy around mid-December and did not start my chemotherapy until January 2018, which would last for 10 months. Each time I had to go for chemo it was long and drawn out. Arriving around 10am and not getting home until six/seven pm. Again, my wife and I discussed all this and again we were very positive and just stuck at it and got it done. I had a few issues with the chemo such as rashes, coughing and just feeling not well at all, but I took that as I knew others were worse off than me.
Going Forward
I believe that positivity has played a huge part in my recovery. I am a firm believer that if I had lay down and not fought this terrible disease, along with the support from family and friends, I would not be here today telling this story, in support for ‘Time to Bring Awareness to Brain Cancer’.
Going forward from 2017, I still have a few issues that have remained, but I will always say, I could have been worse. Waking up every morning is a massive bonus which I am forever grateful for.
I know that the NHS gets a lot of bad publicity for one thing or another, but I can honestly say that these people have made my life a lot better than it could have been, and I will be forever in their debt. The professionalism and care of all staff has helped me and my family get on with our lives.
Whenever my wife and I were going through all these procedures, surgery, treatment etc, I had to take a year of work and at the time I was working for DFI. I have to applaud the department for the support I had throughout the process, and even now I still have to attend MRI scans every 6 months which involves time off work.
This has been hard for me to write but it shows that you can come through at the other end. Since 2017 I have changed roles within the NICS, been promoted and just in last few weeks
‘my wife and I adopted the most beautiful little girl’.
I have been asked by a few people how I went through everything, it is quite simple, you have no other choice. If I had to give advice to anyone going through this I would say, what has happened has happened, you have no reverse in your car so just go forward, nothing you can do back there. You know your body better than anyone.
I really hope that by sharing my story, I can help people going though any cancer diagnosis.
Thanks for taking the time to read my story.
Paul
